Introduction
The secondary cleft lip nasal deformity presents an extreme challenge to the facial plastic surgeon. The deformity is complex and involves all tissue layers, including skeletal platform, inner lining, osseocartilaginous structure, and overlying skin. It is often the characteristic cleft nasal deformity that is noticeable to the observer after a well performed cleft lip repair.
Secondary repair of the cleft lip nasal defect requires an understanding of the pathological nasal anatomy associated with congenital clefting. The basic cleft nasal deformity is characteristic and defendant upon the original extent of clefting of the lip. However, the secondary nasal defect varies greatly and is a result of: 1) the original malformation, 2) any interim surgery performed, and 3) growth of the nose and face. The cleft surgeon must therefore have a treatment philosophy and technique flexible enough to reconstruct a variable range of associated nasal problems. This chapter describes the pathological anatomy associated with cleft deformities, and describes approaches and techniques designed to improve form and function of the cleft nose.
Anatomy of the Unilateral Cleft Nasal Deformity
The etiology of the primary unilateral cleft nasal deformity is a lack of skeletal support of the cleft alar base. The unilateral cleft malformation also includes a hypoplastic and malaligned orbicularis oris muscle on the involved side. The combination of the lack of cleft side skeletal support and abnormally oriented muscle results in a characteristic caudal deviation of the nasal septum to the noncleft side (Figure 1). Lack of muscular continuity often is associated with an abnormal configuration of the cleft nasal sill. The unilateral cleft side nasal base is lateral, posterior, and inferior to its noncleft counterpart alar base.
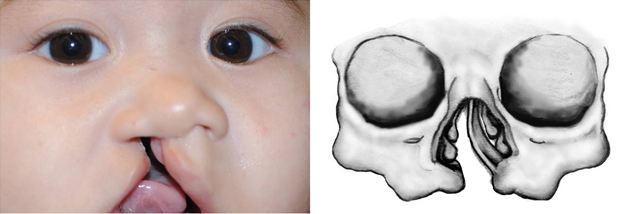
Figure 1. Classic deviation of caudal septum to the non-cleft side.
Inadequate skeletal support to the cleft alar base causes asymmetry and displacement of the cleft lower lateral cartilage (LLC) (Figure 2). The medial crus of the cleft LLC is shorter than the noncleft LLC, while the lateral crus of the cleft LLC is longer than its noncleft counterpart. The cleft side dome is wide and the tip is relatively underprojected on the affected side. Although underprojection of the nasal tip accompanies the unilateral cleft lip, the amount of the underprojection is less than it is in bilateral clefts. There is always asymmetry of the nasal tip and the alar base; the extent of the asymmetry is related to the extent of the original deformity.
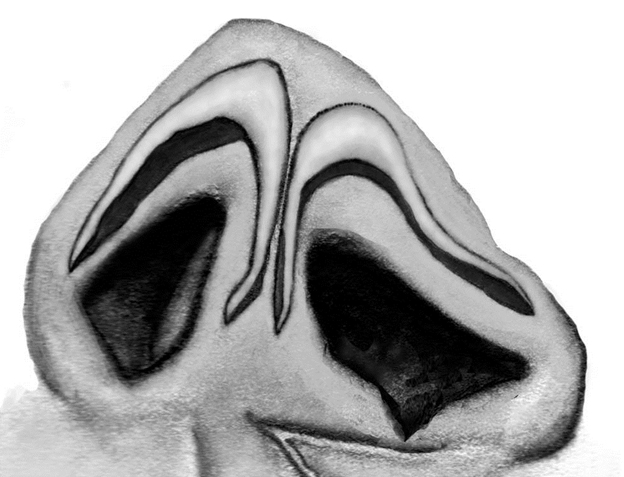
Figure 2. Illustration of lower lateral cartilage and alar base asymmetry.
Anatomy of the Bilateral Cleft Nasal Deformity
The nasal deformity associated with bilateral cleft lips is usually more symmetric than is the unilateral nasal deformity. Nasal asymmetry in bilateral clefts is only present if significant differences exist in the severity of the lip clefting. The bilateral nasal deformity usually includes a deficiency in skin and soft tissue between the vermillion-cutaneous junction of the lip and the nasal tip. This results in a short columella and underprojection of the nasal tip. The extent of the underprojection of the tip is related to the amount of projection of the premaxilla and the underlying skeletal deformity.
The nasal tip in the bilateral deformity is broad and flat. Both medial crura of the LLC are shorter than normal, while the lateral crura in bilateral clefts are longer than normal. The nasal septum in bilateral clefts is usually in the midline, but the septum is often wide and reduplicated. The alar bases are poorly supported due to skeletal deficiency, and this causes lateral and posterior malposition of both the cleft alar bases.
Primary Management of the Cleft Nasal Deformity
Traditional management of the cleft lip deformity often does not focus attention on the nose. However, it is clear that early management of the nasal deformity minimizes nasal asymmetries and allows the nose to grow in a symmetric fashion. Primary treatment of the cleft nasal deformity includes pre-surgical nasoalveolar molding (PNAM) and primary rhinoplasty (at the time of lip repair).
PNAM is a continual low-level pressure on the cleft alveolar segments. This non-surgical technique is initiated before one month of age and exerts a measurable orthopaedic effect. Non-surgical repositioning of the bony cleft segments helps to: 1) narrow the cleft gap, 2) improve alar base symmetry in asymmetric clefts, 3) expand the soft tissue envelope, and 4) elongate the columella.
Although PNAM is not used in all clefts, the technique is very helpful in wide clefts with significant asymmetry. In bilateral clefts with a “locked-out” premaxilla, PNAM can facilitate retropositioning of the premaxilla, allowing a single stage definitive cleft repair. Successful use of PNAM requires a team approach with a dedicated orthodontist, and a compliant and understanding family (Figure 3).
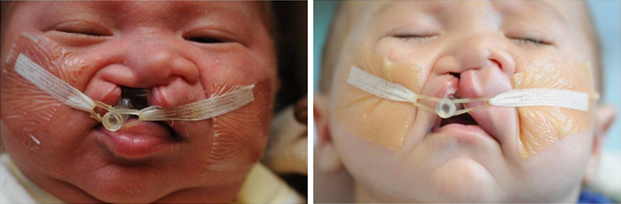
Figure 3. The effects of 6 weeks of PNAM (from left to right).
Primary Cleft Nasal Repair
Various philosophies and techniques of primary cleft rhinoplasty have been described. Approaches usually include some form of caudal septal repositioning and nasal tip reorientation. Most cleft surgeons do not advocate removal of cartilage in early childhood, but rather use repositioning of cartilage with suture techniques. These maneuvers can usually be accomplished with the standard incisions used to close the lip cleft.
After the lip incisions are made and the primary lip dissection is completed, the muscle and soft tissues of the alar base are separated from their maxillary attachments. The malpositioned alar base is freed by creating an internal alotomy at the anterior head of the inferior turbinate (Figure 4). If adequate soft tissue dissection of the alar base is performed, the cleft alar base can be repositioned (during closure) in the optimal 3-dimensional position.
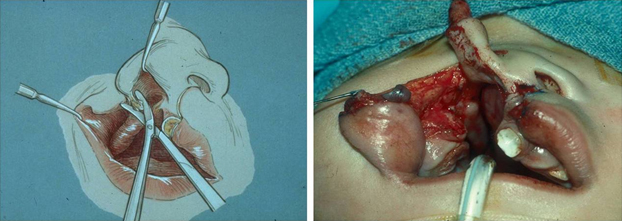
Figure 4. Alotomy being performed to reposition the alar base.
The cleft side LLC is then dissected from its cutaneous attachments by creating a medial and a lateral tunnel (Figures 5 and 6). These subcutaneous tunnels are connected and allow the cleft LLC to be repositioned into a more symmetric fashion. Care is taken to not violate the vestibular skin, avoiding the complication of secondary adhesions and nostril stenosis.
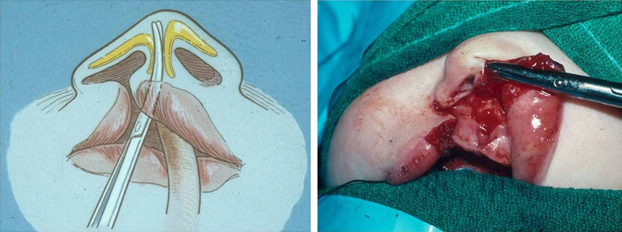
Figure 5. The cleft side medial crura is dissected from its cutaneous attachments.
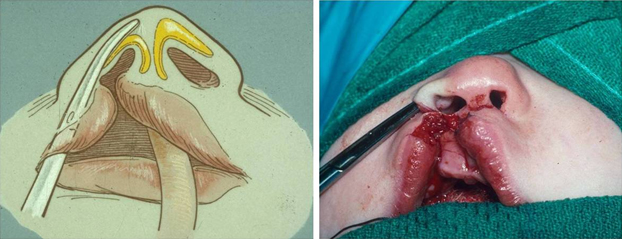
Figure 6. The cleft side lateral crura is dissected from its cutaneous attachments.
Primary cleft rhinoplasty begins with closure of the nasal floor and sill. This closure is first started with reapproximation of the musculature of the nasal base. The skin of the nasal sill is then closed with attention paid to making the cleft nasal sill look like the noncleft side. Closure of the nasal sill is performed with # 5-0 chromic catgut suture. It is important to not narrow the sill too much. A nasal base which is too wide is easy to narrow secondarily, while a too narrow sill is difficult to widen.
The other component of primary cleft rhinoplasty is to reposition the cleft nasal tip into a more projected, symmetric position. Many surgeons have been reluctant to perform rhinoplasty at the time of lip repair to avoid theoretic growth inhibition of the nose. However, McComb and Coughlan have observed no nasal or facial growth inhibition in patients followed for 18 years after undergoing primary cleft rhinoplasty. The initial alar base and tip symmetry obtained in their patients was obtained during the entire study period.
After the nasal sill is reestablished and the lip is repaired in a layered fashion, the cleft LLC is repositioned to create a narrowed, projected location. This is achieved with internal mattress, or tie-over external bolsters. A new dome occurs, with a lengthened medial crus and a shortened lateral crus (Figure 7). If nasal bolsters are used, they are removed in 7 to 10 days. The resulting nasal tip is more symmetric, defined, and projected.
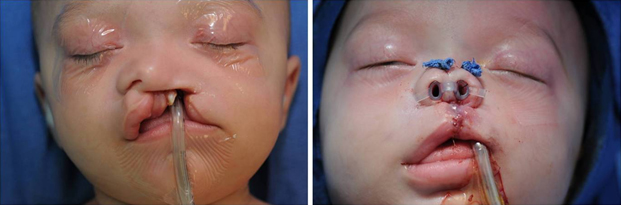
Figure 7. Pre and post primary cleft rhinoplasty.
Secondary Cleft Septorhinoplasty
The timing of definitive septorhinoplasty in cleft patients should take into consideration both psychological aspects and physical growth maturation of the nose and the overall facial skeleton. In cleft patients with significant malocclusion and dentofacial deformity (usually class III secondary to maxillary hypoplasia), definitive nasal reconstruction is usually delayed until after the orthognathic surgery is completed (Figures 8 and 9). This often postpones the surgery until 17-18 years of age in females and until 19 years in males.
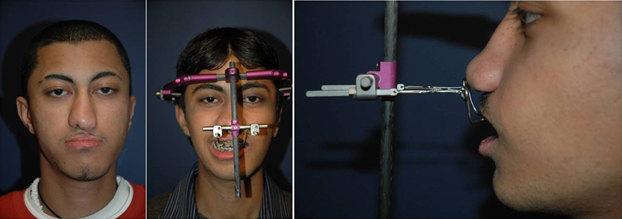
Figure 8. Patient with unilateral cleft lip and maxillary hypoplasia. LeFort I osteotomy with distraction osteogenesis being performed prior to secondary cleft rhinoplasty.
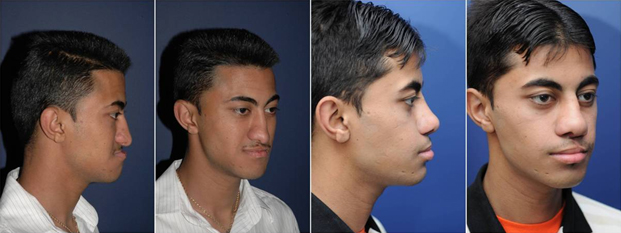
Figure 9. Before and after LeFort I osteotomy with distraction osteogenesis and subsequent secondary cleft rhinoplasty with autologous costal cartilage.
The goals of definitive nasal surgery are to maximize nasal function and appearance. This requires total septal reconstruction, and often necessitates significant cartilage grafting for support and camouflage of deformities (Figures 10 and 11).
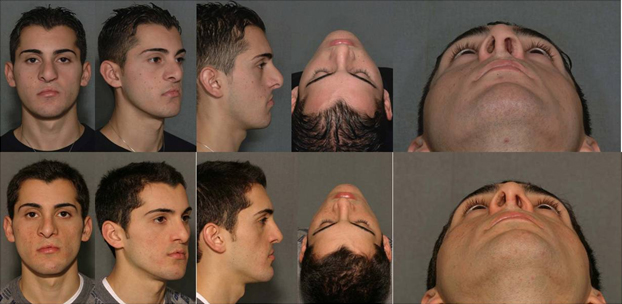
Figure 10. Secondary cleft rhinoplasty (preop above, postop below).
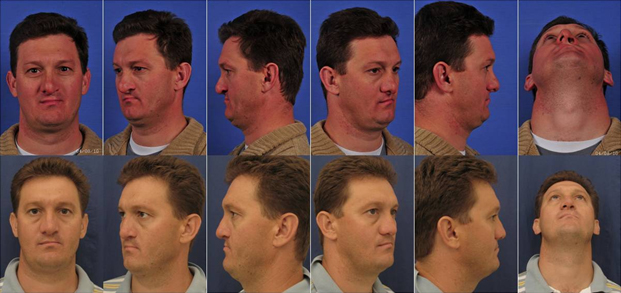
Figure 11. Secondary cleft rhinoplasty (preop above, postop below).
Incisions and Approaches
Both endonasal and external approaches can be used for cleft septorhinoplasty. The open, or external approach is usually preferred as this approach allows superior visualization for diagnosing deformities, and better exposure for suturing structural grafts. In addition, the open approach provides excellent access to the caudal septum, which is usually significantly deviated and poorly supported.
If the skin and columellar soft tissues are adequate, a standard columellar incision (either a stairstep or an inverted notched-V) is utilized. However, if inadequate skin and soft tissue exists, recruitment of columellar skin is required. In the unilateral cleft deformity, an asymmetric V-to-Y is used. In the bilateral deformity, a midline V-to-Y or forked flaps can create additional columellar soft tissue necessary to increase projection.
Septal Reconstruction
The nasal septum associated with cleft deformities is often severely deviated, with the caudal septum deflected to the noncleft side, and the posterior septum bowing into the cleft side. In order to reconstruct the cleft septum, complete mobilization of the caudal septum must be performed. Access graft to its caudal border (Figure 12). This can be performed in an overlapping fashion to the cleft septum is usually obtained through an open approach, by separating the intracrural ligament between the feet of the medial crura of the LLCs. After detaching the caudal septum from its maxillary attachments, the septum is usually strengthened by affixing a cartilage, or the cartilage graft can be sutured end-to-end.
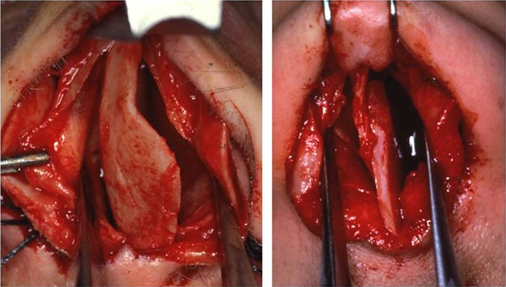
Figure 12. Correction of the deviated septum in the unilateral cleft lip patient.
The posterior septum is then straightened with standard incisional and excisional
techniques. Once the septum is straightened and adequately supported, the anterior portion is sutured to the anterior nasal spine with long-acting resorbable monofilament suture. The well-supported septal construct is then used as a platform upon which to anchor the nasal tip complex.
Cleft Rhinoplasty
After the nasal septum is stabilized and repositioned, the outer nasal structure can be reconstructed. This usually requires structural grafting to support the underprojected and inadequately supported cleft side infrastructure. The cartilage grafts are obtained from the posterior septum, the conchal bowl of the ear, and the rib. In most instances, sufficient graft material can be harvested from the septum. In secondary cases, however, costal cartilage is often required for adequate supporting cartilage.
Upper Nasal Third
The upper one-third of the nose is usually not affected by the cleft malformation. Standard nasal osteotomies, lateral +/- medial, are performed to narrow the nose, close an open roof deformity, or to straighten a deviated nasal pyramid. It is important to expect a weak middle third on the cleft side. This will, of course, affect the method and type of osteotomy performed.
Middle Nasal Third
The middle nasal third in patients with clefts is usually weak as a result of inadequate skeletal support on the cleft side. Reconstruction of the cleft side middle third can be performed with a spreader graft (placed between the upper lateral cartilage (ULC) and the nasal septum, an onlay cartilage graft, or flaring sutures. In some instances, more than one technique can be used (e.g. flaring sutures and spreader grafts). Spreader grafts are frequently used bilaterally, and can be placed in an asymmetric manner (Figure 13). In bilateral cleft nasal deformities, bilateral spreader grafts are often used.
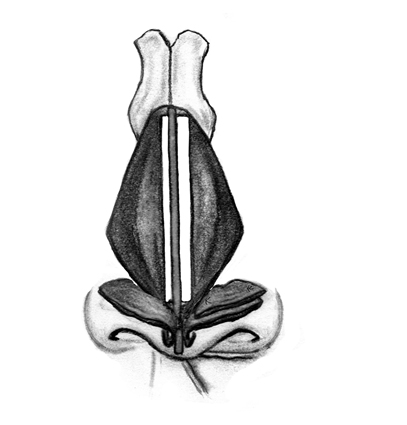
Figure 13. Placement of asymmetric spreader grafts.
It is important to anticipate functional consequences from bony or cartilaginous hump reduction in cleft patients. The underlying weakness in skeletal support (secondary to the alveolar bony cleft) of the cleft side alar base results in a deficient platform supporting the lateral nasal soft tissues. This bony weakness, along with the significant underlying septal deformity, predisposes the cleft patient to nasal obstruction. For this reason, any patient with short nasal bones or weak ULCs requires support in the middle nasal third.
Lower Nasal Third
The lower third of the nose always exhibits some abnormality in patients with congenital clefts of the lip. In patients with unilateral clefts, there is always some asymmetry of the alar base and nasal tip. In patients with bilateral deformities, there is lack of normal tip projection and flaring of the lateral crura of the LLCs. These deformities can be partially corrected with primary rhinoplasty. However, residual secondary deformities of the nose almost always are present. For this reason, all patients and families should expect to have definitive secondary septorhinoplasty.
The caudal nasal septum is stabilized with structural grafting (either extended spreader grafts or a septal extension graft) and repositioned into the midline. The nasal tip can then be positioned into the optimal 3-dimensional position by suspending the tip complex to the caudal septum. The cleft side LLC is advanced anteriorly, creating improved tip projection on the cleft side. This advancement equalizes and defines the nasal tip. After creating improved nasal tip projection and symmetry, a nasal tip graft can be fashioned and sutured-in-place to further increase projection and camouflage any residual asymmetry.
Treatment of the Malpositioned Alar Rim
The cleft LLC is poorly supported and always malpositioned. This malposition results from lack of alar base support. The contour of the lateral crus of the LLC is concave, as opposed to the normal (noncleft) relative convexity. Additionally, the lateral crus is typically inferiorly displaced, or hooded.
Treatment of the hooded lateral crus of the LLC can be performed by suturing the superior, or cephalic edge of the LLC to the periosteum of the ipsilateral nasal bone. Restoring the normal convexity to the lateral crural contour can be achieved with several methods. These include: 1) using the lateral crus as a free graft and flipping the concave cartilage into a convex position, 2) alar strut grafts, 3) alar rim grafts, or 4) onlay camouflage grafts (Figure 14). At the conclusion of the alar rim repositioning, maximal 3-dimensional alar base and tip symmetry should be present.
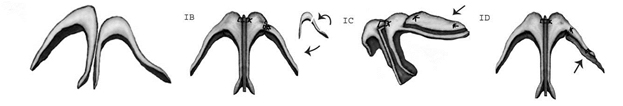
Figure 14. Use of resection, repositioning, and grafting techniques to correct the asymmetric lower lateral cartilages.
Summary
The cleft nasal deformity is extremely challenging and presents both functional and aesthetic problems. The tissue deficiencies associated with congenital clefting of the lip and palate involves all tissue layers, from the skeletal framework to the skin. Primary rhinoplasty can help minimize the secondary deformity and allow more symmetric nasal growth. However, most patients have significant secondary aesthetic and functional nasal problems, requiring complex nasal reconstruction. If the patient has an associated dentofacial deformity requiring orthognathic surgery, this bony surgery should be completed prior to rhinoplasty surgery.
Secondary septorhinoplasty is performed after full nasal growth is completed. Attention should be paid to adequate straightening and support of the nasal septum. Nasal surgery usually requires structural grafting to the middle and lower nasal thirds. Structural grafting will enable the surgeon to maximize nasal function and aesthetics.
References:
- McIndoe A, Rees TD. Synchronous repair of secondary deformities in cleft lip and nose. Plast Reconstr Surg 1959;24:150-161
- Sykes JM, Senders CW. Pathologic anatomy of cleft lip, palate, and nasal deformities. In: Meyers AD (ed). Biological basis of facial plastic surgery. New York: Thieme Medical Publishers, 1993:57-71
- Latham R. The pathogenesis of the skeletal deformity associated with unilateral cleft lip and palate. Cleft Palat Craniofac J 1969;6:404-414
- Jablon JH, Sykes JM, Nasal airway problems in the cleft lip population. Facial Plast Surg Clin North Am 1999;7:391-403
- Stenstrom SJ. The alar cartilage and the nasal deformity in unilateral cleft lip. Plast Reconstr Surg 1996;38:223-231
- Park BY, Lew DH, Lee YH. A comparative study of the lateral crus of alar cartilage in unilateral cleft lip nasal deformity. Plast Reconstr Surg 1998;101:9150919
- TerKonda RP, Sykes JM. Controversies and advances in unilateral cleft lip reair. Curr Opin Otolaryngol 1997;5:223-227
- Sykes JM, Senders CW. Surgery of the cleft lip nasal deformity. Oper Techn Otolaryngol Head Neck Surg 1990;1:219-224
- McComb HK, Coghlan BA. Primary repair of the unilateral cleft lip nose: completion of a longitudinal study. Cleft Palate Craniofac J 1996;33:23-31
- Sykes JM, Senders CW. Surgical treatment of the unilateral cleft nasal deformity at the time of lip repair. Facial Plast Surg Clin North Am 1995;3:69-77
- Salyer KE. Primary correction of the unilateral cleft lip nose: a 15-year experience. Plast Reconstr Surg 1986;77:558-566
- Sykes JM, Senders CW, et al. Use of the open approach for repair of secondary cleft lip-nasal deformities. Facial Plast Surg Clin North Am 1993;1:111-126
- Toriumi DM, Johnson CM, Jr. Open structure rhinoplasty. Facial Plast Surg Clin North Am 1993;1:1-22
- Fisher DM, Mann RJ. A model for the cleft lip nasal deformity. Plast Reconstr Surg 1998;101:1448-1456
- Madorsky SJ, Wang TD. Unilateral cleft rhinoplasty: a review. Otolaryngol Clin North Am 1999;32:669-682
- Millard DR, Morovic CG. Primary unilateral cleft nose correction: a 10 year follow-up. Plast Reconstr Surg 1998;102:1331-1338
- Sykes JM. The importance of primary rhinoplasty at the time of initial unilateral cleft lip repair. Arch Facial Plast Surg 2010;12(1):53-55
