1. INTRODUCTION
History of rhinoplasty comes from many centuries ago, most probably from ancient cultures in Egypt. One of the most important steps in modern open-tip rhinoplasty history was taken in 1921 by Rethi, from Budapest, which described an external approach to expose alar cartilages and nasal dorsum only through a unique high columellar skin incision, connected with bilateral endonasal skin incisions along the caudal border of the alar cartilages.(1) The Rethi incision became the dictum for transcolumellar approach.
Later on, Haubenrisser(2) in 1956 modified the Rethi incision with propose of facilitating the flap elevation. He described the extension of the incision laterally to the alar facial junction, curving it in the crease of the alar facial junction over the external skin.
Sercer(3) tried to optimize the Rethi incision and described a horizontal mid columellar incision. He also introduced the term “decortication of the nose” to define the exposition of the nose respecting the anatomic structures (e.g. no incisions on cartilages).
Padovan(4), who worked with Sercer, modified is incision and created a V-shaped incision located at the natural crease caused by diversion of the foot plates of the medial crura. He also highlighted the preservation of the perichondrial and periosteal layer over the nasal dorsum.
Goodman(5) after getting to know Padovan`s work, started to apply the external approach in is rhinoplasty in a systematic manner. He formulated the potential values of the external approach and refined the incision, also known as “Butterfly” or “Gull-wing”. Goodman described an interrupted, broken line mid columellar skin incision. He also introduced some innovations to the whole open rhinoplasty procedure, such as the use of electro cautery to minimize blood loss and the use of a rotating burr to sculpt the nasal dorsum.
The concept of “open structure rhinoplasty” was presented by Johnson, an associated of Anderson and Toriumi.(6) This author combined the external approach with the concept of autologous cartilage grafts to the nasal tip, based on the previous work of Sheen(7), and he gave the most emphasis to a strong structural support of the nose.
Open-tip rhinoplasty, also known as external approach or open structure rhinoplasty, has gained much popularity in the past three decades among rhinoplasty surgeons due to some main features of this technique, such as direct visualization of the anatomy and precise diagnosis of the deformities, bimanual control of the structures and possibility of electro cautery hemostasis. Another important characteristic of the open approach is the ability to show and teach this technique to the younger trainees or fellows (Table 1). Exposure is a basic principle in any surgery, but gains an extra emphasis in aesthetic and reconstructive surgery.
| Open Approach | Closed Approach | |
| Advantages | Complete anatomic exposition | Less surgical dissection therefore less edema |
| Precise intraop diagnosis of the structural alterations | Less postop edema | |
| More predictable results | Less risk of cicatricial changes | |
| Better for teaching youngsters | Shorter surgical time | |
| Shorter period of convalescence | ||
| Disadvantages | Longer Operating Time | Identification of the anatomical structures |
| More need of using grafts | Not suitable for all patients (e.g. patients with great asymmetries, patients with complex nasal tip deformities, etc.) | |
| Columellar Scar | ||
| Longer convalescence |
Table 1 – Advantages and disadvantages of the different approaches
Although excellent results are achieved by experienced surgeons, for many, closed rhinoplasty remains a difficult technique with a long learning curve.
The open approach rhinoplasty can be used in almost any clinical case, depending on the surgeon’s experience and preference.
Modern concepts in soft tissue surgery favor an interrupted midcolumellar skin incision for good cosmetic results. The incision is made parallel to the relaxed skin tension line, in an interrupted fashion which redistributes the wound`s contractile force.
2. BRIEF SURGICAL ANATOMY
The nose is formed by the combination of the bony vault, the cartilaginous structure and soft tissue covering it. Two thirds of the nose is constituted by cartilage. The bony vault is formed by the nasal bones and the ascending processes of the maxilla. The nasal bones articulate with the frontal bone and the ascending process of the maxilla. The upper and lower alar cartilages, and the anterior half of the septum constitute the cartilaginous portion of the nose structure. The upper alar cartilage forms the midvault or middle third of the nose and articulates with the lower alar cartilage at the scroll area. The lower third of the nose is formed by the caudal septum and the lower lateral cartilage.
The tripod concept explains the tip dynamic and helps the surgeon to understand the effect of is actions on tip rotation and projection. The two medial crura of the lower lateral cartilages act as one leg of the tripod. The two lateral crura form the other two legs of the tripod. This way, tip rotation and projection can be managed by changes in the pivot point of the tripod.(8)
The superficial muscloaponeurotic system (SMAS) it`s a layer of fibrous and muscular tissue that connects and sheaths the muscle of facial expression. The SMAS divides the subcutaneous fat into 2 layers.(9) Also it sends out fibrous septa that run perpendicularly through the fat to insert into the overlying dermis, acting as a network that transmits contractions of the facial muscles to the skin. The SMAS serves as a guide to perform dissection and mobilization of the tissues along appropriate planes, protecting the nerves and the blood supply that run bellow it. It is also very important to preserve the SMAS in rhinoplasty because it can camouflage bony and cartilaginous irregularities.
The nasal musculature is divided in three major groups: the elevator, depressor and the compressor. The elevator muscles include the procerus and the levator labii alaeque nasai. The depressors include the ala nasalis and the depressor septi nasi. The compressor muscles include the transverse nasalis and the compressor narium minor.
The nasal framework has a good vasculature provided by vessels from both the external and internal carotid system. There are a lot of collateral vessels between the branches of the Ophthalmic Artery (external nasal a., dorsal nasal a., anterior ethmoidal a.) and the branches of Facial Artery (angular a., superior labial a., columellar a., inferior and superior alar a.).
The area of the nose more prone to vascular suffering is the nasal tip. Vascular supply and lymphatic drainage are found superior to the nasal musculature. This way we have to be especially careful on soft tissue removal when reshaping the nasal tip.
The ideal plane is deep to nasal muscle, superficial to the perichondrium and the periosteum; this is an avascular plane that facilitates tissue mobilization and minimizes bleeding.
There is minimal lymphatic drainage in the columellar, therefore the midcolumellar incision in open rhinoplasty causes spare edema.
3. SURGICAL TECHNIQUE
Infiltration
One very important step in open rhinoplasty is the first one: infiltration. It should be done before disinfecting and dressing the patient, in order to take effect for at least 15 minutes and so maximize the vasoconstrictive effect of epinephrine. . Infiltration is done using 8 to 10ml of lidocaine at 1% with epinephrine at 1: 100 000, and is applied in six key points: 1) vertically from the nasal tip to the anterior nasal spine; 2) in the columella, through the nasal vestibulum, perpendicular and anterior to the caudal septum; 3) in the infra tip point parallel to the nasal dorsum; 4) vestibulum, in the intercartilaginous region; 5) through the pyriform aperture, lateral and parallel to the ascending process of the maxilla; 6) along the nasal septum, in the sub mucosal area. After this, cottonwoods pledges soaked in phenylephrine or cocaine ointment at 10%, are placed in both nasal cavities to reduce nasal mucosa, improve exposure and minimize blood loss.
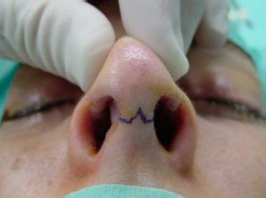 |
| Figure 1- Inverted V |
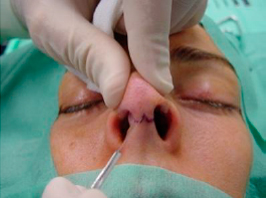 |
| Figure 2- Incision |
Incision/Surgical Technique
Exposure of the nose osteocartilaginous structure is obtained by using a transcolumellar incision that is done at the narrowest part of the mid portion of the columella. In this location there is the support of the lower lateral cartilage (LLC) medial crura, that is very important to minimize scar contraction and is one of the reasons why is so important to preserve intact medial crura. The incision is made parallel to the relaxed skin tension lines, in an interrupted manner so that the wound`s contractile forces are redistributed (figure 1). The authors usually use a number 11 blade to do the inverted “V” incision with a sawing motion (figure 2). Is very important that the blade stays perpendicular to the skin, so that the wound edges are even and the scar formation can be perfect. In the horizontal portions of the columellar incision we use the 15 blade because at this point there aren`t acute angles.
This midcolumellar incision continues laterally with the marginal incisions made on the vestibular skin caudal to the lower border of the medial and intermediated crura, just 2mm behind the leading edge of the columellar.
The next step is to use the Converse scissor to dissect under the muscle-aponeurotic plane. To do so one as to introduce de Converse scissor by one of the columellar portion of the marginal incisions and dissect superficial to the caudal margin of the LLCs and tunneling through until reaching the contralateral marginal incision (figures 3 and 4).
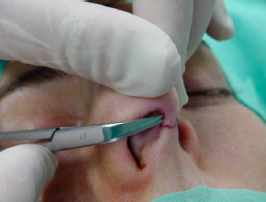 | 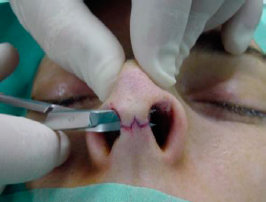 | |
| Figures 3 and 4- Dissection with Converse scissor. |
To avoid damaging the skin flap and the caudal margin of the medial crura we ordinarily use the Converse scissor to protect them while completing the incision with the 15 blade in a secure way (figures 5 and 6).
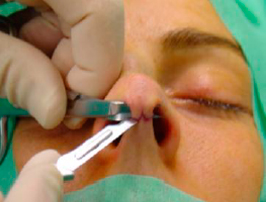 | 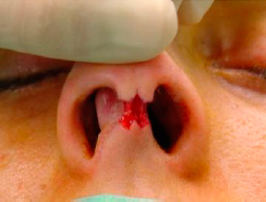 | |
| Figures 5 and 6- Completing the incision while protecting the medial crura. |
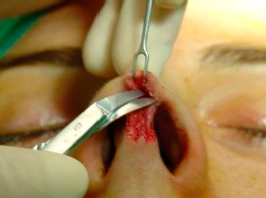 |
| Figure 7- The supraperichondrial plane |
The columellar skin flap is elevated superficial to the medial crura with blunt and sharp scissor dissection, leaving as much soft tissue as possible on the skin flap. The dissection must be as close to the cartilage as possible, avoiding damages to the superficial muscloaponeurotic system (SMAS). This enhances the viability of the skin flap.(9) Another important reason for one to dissect in the correct plane is that the perichondrial plane is relatively bloodless and this way is possible to get an almost bloodless surgical field.
After correct identification of the caudal margins of the medial cruras, progress dissecting in the supraperichondrial plane, over the margin and the medial surface of the intermediate and lateral crura of the LLC (figure 7). For better surgical exposure of the domus area is
necessary to use two tension points: on the intermediate crura, with a delicate double hook, where the assistant surgeon applies lateral and downward tension, while the main surgeon exposes this area with upper tension by a Cottle retractor, pulling the flap and the indicator finger backed on the nasal dorsum. Dissection continues caudally in the domus area (figures 8, 9 and 10).
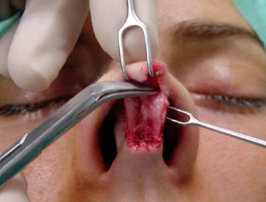 | 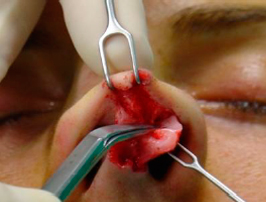 | 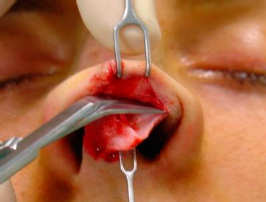 | ||
| Figures 8, 9 and 10 – Dissection of the nasal tip in the supraperichondrial plane. |
As the surgeon dissects laterally the LLC, in the supraperichondrial plane, he also viagra online cheap completes the marginal incision with the converse scissor. This way he can correctly identify the caudal margin under direct vision and avoid trauma to the cartilage (figures 9 and 10).
Progress dissecting laterally and cephalic until full dissecting and expose all the LLCs and identify the anterior septal angle (figure 11).
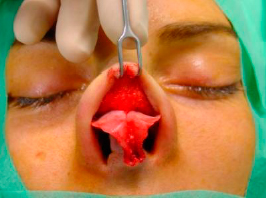 |
| Figure 11- Full exposer of the nasal tip. |
When the nasal tip is exposed the surgeon must go on and start dissecting the cartilaginous structure of the nasal dorsum, proceeding dissection cephalic in the subaponeurotic and supraperichondrial plane over the medial aspect of the upper lateral cartilages (ULC). Elevate de SMAS in the middle line until the rhinion (figure 12).
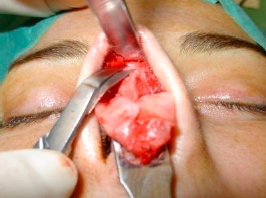 |
| Figure 12- Elevation of the SMAS |
To expose the bony pyramid we incise the periosteum 2mm above the caudal rim of the nasal bones with a 15 blade, and remaining in the subperiosteum plane, we elevate the periosteum using a Joseph elevator, in cephalic direction until we reach the nasion (figure 13), creating two paralateral subperiosteal tunnels and then joining them in midline (figures 14 and 15). Optimal exposure is achieved by raising the flap with an Aufricht retractor.
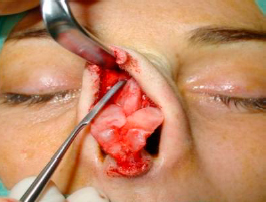 | 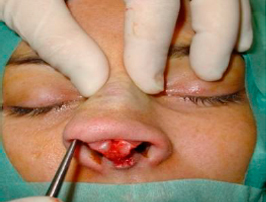 | 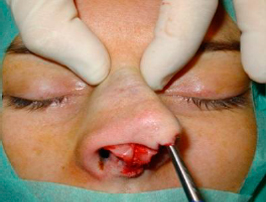 | ||
| Figures 13, 14 and 15 – Elevation of the periosteum until the nasion, with two paralateral subperiosteal tunnels. |
Sometimes we find some midline fibers that difficult the union of the two lateral subperiosteum tunnels, in such case these fibers must be cut with the Converse scissor.
After the entire nasal framework is exposed, we are in a privileged position to address the nasal septum from above. We create a subperichondrial tunnel in both sides, beneath the angle formed by the septum and the ULC, starting in the anterior area and dissecting in cephalic direction, in order to preserve the perichondrium when we have to remove a osteocartilaginous hump or when is necessary to disconnect the ULC from the septum (figures 16 and 17).
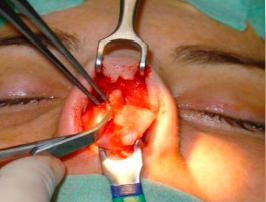 | 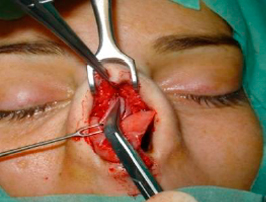 | |
| Figures 16 and 17 – Creation of subperichondrial tunnels, beneath the angle formed by the septum and the ULC. |
When we manage to expose all major nasal structures with this open approach, we can shape them under direct vision.
It isn`t our propose, in this chapter, to approach the different techniques of reshaping the nose, so as it follows we describe how to close our columellar incision.
Closure of the Midcolumellar Incision
It is important to close the incision in two layers. We suture the subcutaneous layer using a polydioxanone (PDS) 5/0 suture, in order to reduce the tension on the cutaneous layer and to enhance skin-edges alignments and slight eversion. Usually it`s only needed one stitch at the midline (figures 18 and 19).
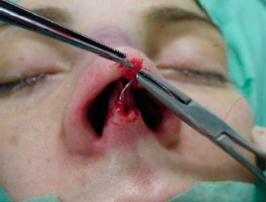 | 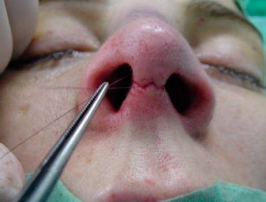 | |
| Figures 18 and 19 – Subcutaneous suture, with PDS stich at midline. |
To close the cutaneous layer we use a 6/0 nylon suture and start with a midline mattress suture at the apex of the inverted V (figure 20). The next two mattress sutures, one on each side, are angled with an oblique and a medial traction to prevent lateral notching of the columellar incision (figure 21). One single suture stich is used to close the vestibular skin at each corner of the columellar flap. This skin alignment is important to avoid any visible notch defect (figure 22).
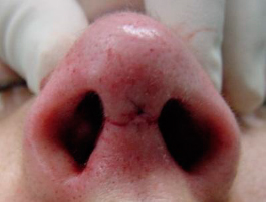 | 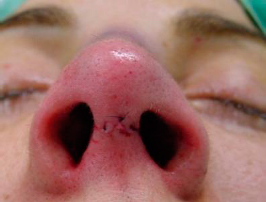 | 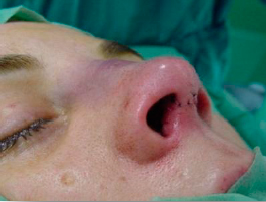 | ||
| Figures 20, 21 and 22 – Final aspect, after closure of the cutaneous plane with nylon 6/0 suture. |
When the columellar incision is made properly and closed meticulously no cosmetic defect of the scar will be visible.
4. BIBLIOGRAPHY
1) Adamson P.A. and Doud Galli S.K., Rhinoplasty Approaches. Arch Facial Plast Surg. 2005, Vol: 7, p. 32-37.
2) Haubenrisser E., Zur Operationstechnik missgestateter und verlagerter Nasenknorpel. I Med kosmet, 1956. Vol. 37.
3) Sercer A. and Mundinhc K., Plastiche Operationen an der Nase un an der Ohrmuschel. Georg Thierne, 1962. Stuttgart.
4) Padovan LF. Combination of extranasal and intranasal approach in surgery of the nasal pyramid and nasal septum (decortication). Can J. Otolaryngol, 1975. Vol: 4, p. 522-528.
5) Goodman W.S. and Charles P.A., Technique of external rhinoplasty. I. Otorhinolaryngol, 1978. Vol: 7, p. 13-18.
6) Johnson Jr C.M. and Toriumi D.M, Open Structure Rhinoplasty. W.B. Saunders, 1990. Philadelphia.
7) Sheen J.H. and Sheen A., Aesthetic Rhinoplasty (ed 2). Cv Mosby, 1978. St. Louis.
8) Toriumi M.D. and Becker D. G., Rhinoplasty Dissection Manual. Linppicott Williams & Wilkins, 1999. Philadelphia.
9) Samaniego E., Prada C., Rodríguez-Prieto M.Á., Surgical Planes of the Head and Neck. Actas Dermosifiliogr., 2011. Vol:102, p. 167-174.
Figures 20, 21 and 22 – Final aspect, after closure of the cutaneous plane with nylon 6/0 suture.
