Abstract
The tenets of rhinoplasty focus on restoring or maintaining the strength and support of the nasal skeleton while altering the contour to achieve the desired aesthetic result. The debate continues unabated over the advantages and disadvantages of an open versus a closed endonasal approach. The open technique offers the obvious benefit of direct observation, which often outweighs the commonly-cited disadvantage of transcolumellar incision and scar. The enhanced exposure is especially beneficial for work on the nasal tip, dorsum and septum and additionally, offers the best possible teaching tool for the trainee. The goal of this chapter is to provide the reader a logical and systematic road map upon which to manage the surgical correction of nasal deformities with the open rhinoplasty approach.
Introduction
Literature suggests that Rethi first introduced the high transcolumellar incision for tip modification in 1921 [1]. In 1957, Sercer extended the incision and described ‘‘nasal decortication’’, defining it as a temporary separation of the nasal skin from the nasal pyramid [2]. Open rhinoplasty subsequently fell out of favor until Padovan, Sercer’s student, presented his series in the early 1970s, reporting the use of the open approach to the septum [3]. Andersen and Wright are generally credited with popularising the open rhinoplasty approach and combining its use with open septoplasty techniques [4, 5] .
Indications
The open rhinoplasty approach allows definitive diagnosis of underlying nasal deformities, particularly in the region of the caudal, superior and dorsal septum, premaxillary spine and lobule. Assessment of the osseocartilaginous framework is especially important in revision surgery. It provides enhanced access to perform precise structural modifications with graft placement and osteotomies. Tip projection may be controlled and refined, such that less dorsal reduction may then be required. Furthermore, scar tissue and redundant subcutaneous tissue may be cautiously excised more easily under direct vision. The delicate valve region can be well- protected, whilst the absence of intercartilaginous incisions reduces the risk of possibility of subsequent nasal valve obstruction due to scar formation and disruption of one of the important tip support mechanisms. The open approach is also ultimately an excellent tool for training and educational purposes [5].
Indications for open rhinoplasty therefore include the following [6]:
- Nasal tip modification, such as bulbous, over/underprojed tip
- Revision rhinoplasty
- Post-traumatic severe external nasal or septal deformity
- Correction of nasal valve dysfunction
- Repair of septal perforations
- Augmentation rhinoplasty requiring multiple grafts
- Cleft lip and palate nasal deformity
- Thin skin where accurate sculpting and camaflage is important
- Some casese of thick nasal skin
The contraindications of the open approach include [7]:
- Intranasal substance abuse (eg. cocaine)
- Psychological or psychiatric instability
- SIMON (single, immature, male, overly expectant, narcissistic) personality traits
- Preoperative diagnosis of nasal dysfunction (with or without aesthetic deformity) that may be better treated with a closed approach (ie. septoplasty) or medical management
- Patient refusal of external scar
- Very thick nasal skin in which postoperative edema may be permanent.
Advantages of open approach include:
- Direct observation of nasal anatomy
- Direct access to relevant anatomy to manipulate and correct derformities.
- Excellent teaching tool for rhinoplasty sugeons
Disadvantages of open rhinoplasty include:
- The transcolumellar scar that may heal poorly and become visible
- Potential for columellar flap necrosis
- Extensive dissection of skin off the osseocartilaginous framework with the potential for increased scarring
- Prolonged postoperative nasal tip oedema and numbness
- Longer operative time when compared with endonasal approach
- Post operative suture removal which can be sometimes uncomfortable
Preoperative Assessment
Every patient should be thoroughly assessed on aesthetic and functional criteria with regards to their nose, as well as psychologically, to obtain informed consent with realistic outcomes. This also includes digital photography and morphing to accurately delineate the goals of rhinoplasty in every case. The surgical plan is re-reviewed with the patient at a second appointment before proceeding with the operation.
History
Presenting functional and aesthetic problems, including symptom severity and duration, previous surgical procedures, allergies, medications, including recreational drug use such as cocaine, and a complete general medical history are elicited.
Clinical Examination
A complete physical examination is vital, with specific facial and nasal evaluation concentrating on skin type and thickness, surgical scars, symmetry and overall balance of facial aesthetic units.
Examination of the nasal septum, internal and external nasal valves, turbinates and lining is undertaken, paying attention to the structure and form of the nasal tip and dorsum. A critical factor in planning tip surgery is the inherent strength and support of the nasal tip – the tip recoil. Depressing the tip toward the upper lip provides a quick and reliable test of the ability of the tip’s supportive structure to spring back into position. If the recoil is instantaneous and vigorous and the tip cartilages resist the deforming influence of the finger, more definitive tip surgery can usually be performed without fear of substantial support loss. The size, shape, attitude, and resilience of the alar cartilages can be estimated by ballottement of the lateral crus between two fingers surrounding its cephalic and caudal margins.
Photography
Photographic documentation during preoperative consultation and during and after the procedure should be obtained. The authors recommend high-resolution digital photography of the nose in the anteroposterior, lateral, basal, bird’s eye and three-quarter profile views, against a blue/grey background. Ideally the operating surgeon should perform the phototgraphy to capture all required additional views.
Anaesthesia and Preparation
The procedure is carried out under a general anaesthetic. Local infiltration of 1% Xylocaine with 1:100, 000 adrenaline is used to achieve a complete external and internal nasal block, some hydrodissection as well as vasoconstriction.
Case History
A 52 year old gentleman presented with worsening nasal airway obstruction after suffering an episode of trauma to his nose. His primary concern was to improve his nasal function and he was less disturbed by the external appearance of his nose. Examination revealed significant collapse of the nasal dorsum with complete lack of septal cartilaginous support. The margins of the fractured nasal bones were clearly visible under the skin-soft tissue envelope, separated by a depressed triangular area in the centre. The nasal tip was severely under-rotated and under-projected. The skin-soft tissue envelope was of medium thickness with some amount of scarring affecting the dorsal skin, alar margins and left soft tissue triangle area. The alar base was excessively wide and from the basal view, appeared sausage-shaped with oblong nostrils.



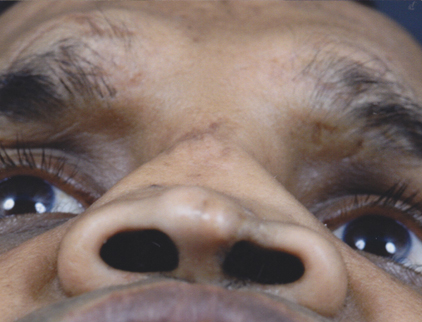
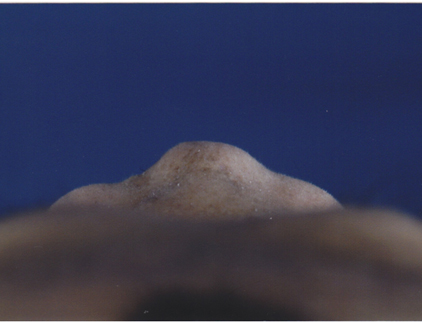
Management Plan:
After detailed discussion with the patient, the surgical decision was to perform an open septorhinoplasty procedure with nasal tip grafting. A rib graft with an L-strut was inserted to rebuild the nasal dorsum, septum and the columella, while subalar struts were used to support the ala. Crushed cartilage was placed on top to camouflage the bone grafts; shield cartilage grafts were also added to the nasal tip. No osteotomies or alar base reduction was done, as aesthetic outcome was not of particular concern to the patient and the subsequent appearance of his nose at this stage was in keeping with his ethnicity. Rim grafts were also inserted to support the alar rim, particularly on the left where there was some retraction.
The Incisions and Exposure
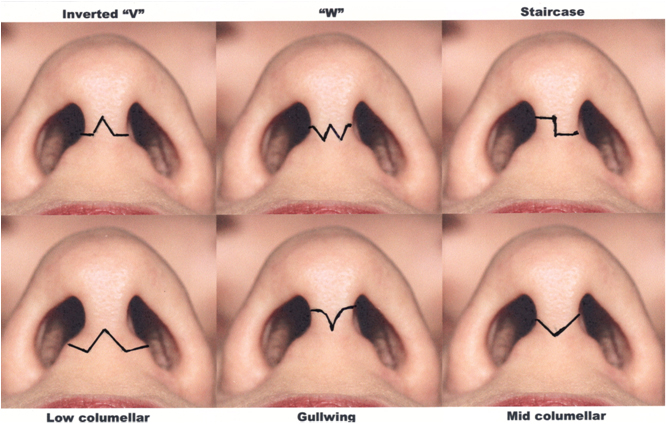
The ideal incision for open rhinoplasty is a mid-columellar incision with break points, avoiding single straight cut across the columella to minimise the risk of contracture. These include inverted-V, W and staircase incisions [8]. In the authors’ experience, the mid-columellar “inverted V” incision made with the 11 blade is desired most. The incision is marked before the infiltration of local anaesthetic. It is important to consider the thickness of the skin on incising, so that the medial crura are not inadvertently incised. Moreover, the incision should be placed above the feet of the medial crura, especially in African and Asian patients who tend to have relatively short medial crura and are hence at greater risk of postoperative transverse columellar notching. The transverse columellar incision part should arc gently around the caudal margin of the medial crura to meet the marginal incisions at 90 degrees. The vertical marginal incisions should be placed slightly behind the true columella to hide it from view, bestowing the advantages of a wider columellar flap, and allowing the natural curve of the medial crus to be followed superiorly with ease.
The columellar flap should be kept as thick as possible, taking care to dissect in the immediate supraperichondrial plane. There may be some brisk bleeding from the inferior columellar artery or branches of the facial artery in the pyriform aperture. This can be controlled with judicious bipolar diathermy to avoid compromising the blood supply to the flap and increasing post-operative oedema. The columellar flap is elevated with tenotomy or Joseph scissors to the superior aspect of the medial crura hugging the border of the LLC. The nasal tip skin is then elevated off the alar cartilages with gentle 3-point traction and scissor dissection. It is important to stay in the immediate supra-perichondrial plane, as a superficial plane of dissection may lead to skin necrosis, as well as exposing minor irregularities post operatively. The nasal dorsum is further exposed by dividing the intracrural ligament and elevating the flap off the osseocartilaginous pyramid in the supraperiosteal plane. The exposure is completed by undermining along the piriform margins and to the upper lateral cartilages (ULCs) as needed.
Logical Steps
In the authors’ experience, the logical sequence of events in open rhinoplasty after performing the incision should follow on with:
- Septal correction
- Nasal tip modification,
- Correction of the dorsal hump and middle third deformities.
- Osteotomies
- The incisions are then closed, and finally alar base reduction is carried out when indicated.
These are discussed in the following section.
I) Septal surgery
Septoplasty is the critical first step of rhinoplasty, offering an early opportunity to harvest septal cartilage for grafting procedures later on, in addition to correcting functional deficits [9]. Dorsal deviations may contribute to internal valve insufficiency and caudal septal deflections may impinge on the external nasal valve, whilst both may lead to a crooked nose appearance.
Open septoplasty provides a superb view of the anterior septal angle. Excellent exposure of the caudal septum is achieved by excising the soft tissue from between the medial crura down to the premaxilla[9]. The nasal spine may be lowered to provide an improved platform for a columellar strut. Submucoperichondrial flaps are elevated bilaterally on either side of the caudal septum, followed by separation of the ULCs from the septum.
Exposure of the septum can be obtained with different techniques, depending on the location of the deviation. In cases where the nasolabial angle needs to be altered, tip projection needs to be altered, large and/or anterior septal deflections; dissection should take place between the medial crura. Here the fibrous attachments of the medial crura are separated until the anterior septal angle is identified. When the septal deflection is located within the central portion of the cartilage, exposure can be achieved with a hemitransfixion or Killian incision. The robust blood supply of the nose allows for a separate Killian incision to be made, even in open rhinoplasty[6].
A severely deviated anterior septum located within the anterior 2 cm of the caudal septum is typically reason enough to open a nose[10]. A noticeable exception to a deviated deflection here would be a straight caudal deflection, which may be more amenable to being repositioned via a swinging door technique to allow the inferior caudal septum to swing freely to the midline and come to rest in the maxillary groove. The cartilage may be scored to liberate it from its intrinsic concavity and convexity patterns. Many anterior septal deflections can be repaired by repositioning the septal cartilage and securing it to the periosteum of the nasal spine, whilst others may require excision and replacement [8].
Another indication for open septoplasty is the deviated dorsal septum which is often difficult to evaluate with the closed approach. A unilateral spreader graft, placed on the concave surface, can provide sufficient strength to help straighten the septum whilst asymmetric spreader grafts may provide further strength[4]. More severe deviations will necessitate an excision and replacement of the deviated component. It is important to recognise a high subradix deviation as it can be a cause of residual dorsal curvature if left uncorrected[9]. This may be treated by vertical shaving of the dorsal septal cartilage and careful mobilisation of the ethmoid plate to the midline, taking care not to fracture it superiorly. Even more significant deviations may necessitate near-total excision and disarticulation of the deviated septum with reconstruction using extracorporeal septoplasty technique. Although the entire septum may be removed, the senior author feels that maintaining a small cartilaginous attachment to the bony septum is a safer and more effective means of repairing septal deviations. Attaching cartilaginous components to bony elements is challenging and can lead to slight shifts in reapproximation, while attaching cartilage to an existing piece of cartilage can lead to improved overall stability.
Patients with ‘‘short’’ nasal septums often benefit from extension of the existing septum. The “caudal extension graft” may be used to adjust septal rotation and projection to help contribute to the position of the nasal tip. In patients with a poorly projected nasal tip, open septoplasty is often necessary to allow for sufficient manipulation of the tip position to adequately project the nose. Some patients with poorly projected noses will have concurrent nasal ptosis and may notice improvement in breathing with restoration of the nose with a more obtuse nasolabial angle[10].
II) Nasal Tip Modification
Shaping of the nasal tip is the most challenging aspect of rhinoplasty surgery. Modification of lower lateral cartilages (LLCs) requires strict maintenance of their symmetry whilst factoring in the eventual effects of healing on the support mechanisms. The “tripod” theory of the nasal tip describes the central leg formed by the conjoined medial crura, and the other 2 legs by the lateral crura, each supported by ligamentous attachments. Alteration of any limb of the tripod hence affects tip position and rotation [11].
Six factors are important in assessing the need for tip remodeling [12]. The surgeon must determine whether the tip requires:
- Reduction in the volume of the alar cartilages
- Alteration in the attitude and orientation of the alar cartilages
- Change in tip projection
- Narrowing of the interdomal distance
- Narrowing of the domal angles and
- Cephalic rotation with a consequent increase in the columellar inclination (nasolabial angle).
This will guide the selection of the most favorable incisions, approach and tip sculpture technique, rather than routine usage of a single method. Ultimately, the key is the symmetry and amount of cartilage retained, readily noted with the open rhinoplasty approach.
IIa) Tip projection
The goals of surgery are to achieve
- Natural looking, well-defined tip to tackle a broad or bulbous nose
- Tip rotation appropriate to gender to address a drooping nasal tip (ideal nasolabial angle is 90 to 105 degrees in males and 100 to 115 degrees in females) and
- Tip projection appropriate to the height of the nasal dorsum and chin.
Enhancement of tip definition can be achieved with suture techniques, cartilage excision techniques or using a combination of two techiques. The former is better suited to a patient with very thin skin, a tip requiring more limited refinement, or a surgeon with less experience, whereas the latter is best reserved for a patient with thicker skin and a surgeon more well-versed with the nuances of excisional techniques.
Cephalic trim. This refers to reduction in the oveall volume of the lateral crura often used to reduce the bulbosity of the tip. A cephalic trim is limited to the more medial aspect of the lateral crus, as trimming the cartilage more laterally will not improve definition more centrally in the lobule and may unnecessarily risk alar collapse by weakening the support that the lateral crura provide to the nasal ala. A minimum height (width) of 6 to 7 mm of the lateral crus should be maintained to ensure adequate alar support and minimize the risk of alar collapse or retraction.
An alternative to cephalic resection of the alar cartilage, for example in the case of a bulbous tip, is a turn-in flap of the cephalic portion of the lateral crus. This enables aesthetic corrections and reinforces the durability of the lateral crus, reduces tip volume and permits medialization of the tip-defining points, thereby achieving a more pleasant-appearing nasal tip[13].
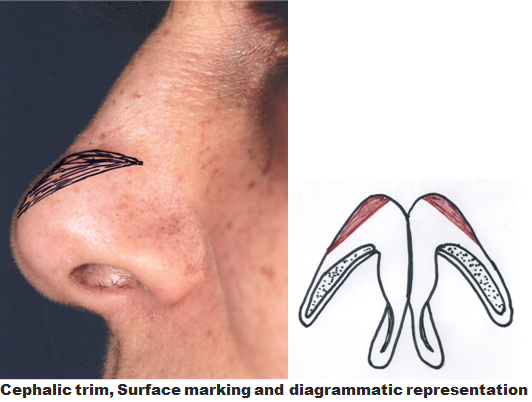
Tip suturing. A broad or bulbous nasal tip may be narrowed by using permanent sutures to modify the lateral crura at the tip (dome). A 5-0 monofilament permanent suture is placed as a horizontal mattress suture spanning the alar dome is the preferred option. The stitch is passed through cartilage only (superficial to the vestibular mucosa underneath) from a point medial to the dome. It exits the cartilage lateral to the dome and is then reinserted back through the cartilage just below the first pass in a lateral-to-medial direction, so that the suture knot ends up between the two medial crura. This is known as a transdomal suture [14]. As the suture is tightened, the domal angle is narrowed, reducing the width of the nasal tip. The same maneuver is repeated contralaterally. At the knot, one limb of the suture from each side is tied to that of the opposite side to unite the two domes from either side to one another (the interdomal suture). This increases stability to the new tip complex, helps maintain the position of tip-defining points and minimizes the effect of soft tissue contracture post operatively.
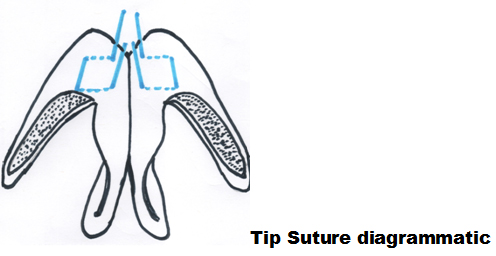
Vertical dome division. This technique is not commonly used in modern rhinoplasty practie, but has its merits when excuted appropriately. Vertical dome division (VDD) describes an excisional technique where the integrity of LLC is interrupted from their cephalic to their caudal border at or near the dome, with preservation of the underlying vestibular mucosa [15]. A cephalic trim is carried out together with excision of a cephalically-based triangle or a wedge of cartilage at the chosen point of “division”. The two medial crura are then sutured to one another several millimeters proximal to the cut edge with 5-0 monofilament mattress suture. This will stabilize the medial crural complex as natural scar contracture develops with healing, minimising the chance of migration or twisting of the cartilage, which might otherwise lead to unsightly irregularities. It is worth noting that excision of a cephalically-based triangle of cartilage lateral to the dome will tend to increase both tip rotation and projection while concurrently narrowing the tip. In such cases the medial border of the excised triangle should be no more than 2 to 3 mm lateral to the dome. On the other hand, a wedge of cartilage can be excised right at the dome, thus shortening the medial and lateral crura equally to effectively deproject and narrow the nasal tip. If additional tip projection is required, strut grafts and plumping grafts may be used as required[16].
IIb) Tip rotation
The planned degree of tip rotation depends on various factors, often including facial balance and proportions, the patient’s aesthetic desires and the surgeon’s aesthetic judgment. Tip rotation and projection are complementary and interrelated. One must also distinguish between true tip rotation and the illusion of cephalic tip rotation achieved by contoured cartilage grafts inserted in the infratip lobule, columella and nasolabial angle.
Cephalic rotation results fundamentally from planned surgical modifications of LLC but might also result from adjunctive procedures on nasal structures adjacent to the alar cartilages. Shortening of the caudal septum, excision of overlong caudal ULCs and septal shortening with a high transfixion incision are used regularly to enhance the effects of a planned degree of tip rotation, which may be facilitated through an open approach [12]. Some basic maneuvers to achieve tip rotation include:
| 1. | Dorsal reduction. A limited reduction (2 to 3 mm) may not result in a significant change in nasal tip rotation but reductions of >4 mm will often result in secondary tip rotation[12]. | |
| 2. | Shortening the caudal septum. In patients with excessive columellar show (>4 mm on lateral view), shortening the overly long caudal septum will promote tip rotation. | |
| 3. | Transdomal/interdomal sutures. Transdomal and interdomal sutures will provide a conservative increase in tip rotation. | |
| 4. | Vertical dome division. When division of the lateral crura is undertaken 2 to 3 mm lateral to the dome VDD, will increase rotation [15]. The medial crura are thus lengthened at the expense of the lateral crura, thereby increasing projection and rotation simultaneously. | |
| 5. | Lateral crural overlay. Vertical division of the lateral crura is performed midway along the lateral crus, and the two segments are then overlapped and suture-fixated. A lateral crural overlay procedure will rotate the tip upward while simultaneously deprojecting the tip (as the lateral crura are effectively shortened) [17]. When tip deprojection is desired together with tip rotation and the nasal tip itself is already narrow and well-defined, maneuvers further out on the lateral crura are preferable to maneuvers executed at the dome itself so that already agreeable tip features are not disrupted. |
III) Grafting Techniques
The open approach is most favorable for reconstructing major framework deficiencies and performing precise graft placement, especially in revision and reconstructive rhinoplasty. The grafts can be easily sculpted and secured under direct vision as desired.
Septal cartilage is the most commonly used grafting material in primary rhinoplasty, due to its straightforward harvest, lack of functional or cosmetic donor site morbidity and reliable long-term results[18]. Septal cartilage can be crushed to provide volume augmentation or soften contour transitions. When harvesting septal cartilage, it is important to maintain a 1.0- to 1.5-cm L-shaped caudal and dorsal strut. Septal cartilage is however often limited in revision rhinoplasty, therefore, the cartilage may be harvested using an open rhinoplasty approach whereby bilateral submucoperiosteal and submucoperichondrial flap elevation is combined with division of the ULCs. Here, the septum and nasal dorsum are laid wide open with unparalleled exposure for diagnosis, harvest of residual structural material and treatment of structural deformities.
Other grafting materials used include auricular cartilage, costochondral (rib) grafts, used for building framework, temporalis fascia and fibroadipose tissue used mainly to camouflage cartilage grafts by softening the framework–soft tissue interface or to correct minor contour irregularities, reducing the risk for graft extrusion, bossae formation and improving the overall quality of the skin envelope[11].
Alloplasts have become increasingly popular due to their ease of use, limitless supply, adaptiability and lack of donor site morbidity. Most alloplasts are polymers and include expanded-porous polytetrafluoroethylene (e-PTFE; Gore-Tex®) [19] and silicone, which is used primarily in Asian patients who have thick skin [18].
Specific grafting techniques suitable for each nasal region will be discussed below.
Grafts in the Nasal Tip:
These may be broadly classified into columellar struts, onlay tip grafts and shield grafts.
i) Columellar struts
The columellar strut is one of the workhorse grafts in rhinoplasty, providing structural support to the nasal tip and improving tip projection. The graft is placed between the paired intermediate and medial crura, through a small vertical incision between the medial crura or through the skin of the nasal vestibule and medial crura on one side. A strong columellar strut is indicated in noses with short, weak, or flared medial and intermediate crura[16]. When using an open rhinoplasty approach, the graft is sutured to the medial crura. Care should be taken to avoid unintentional distortion of the nasal tip contour or the infratip lobule. The graft must be placed short of the domes to avoid excessive prominence with a ‘‘unidome’’ outline. Preserving a small amount of soft tissue over the nasal spine prevents clicking and displacement of the graft with lip movement. For greater stability, the columellar strut may be secured to the nasal spine or premaxilla.
Septal or costal cartilage is recommended, although double-layered auricular cartilage will often provide sufficient strength. Using the perpendicular plate of the ethmoid or other bone grafts may be effective but requires perforation before suturing. In the patient who has a dependent caudal septum requiring increased projection, establishing a tongue-in-groove relationship between the medial crura and the nasal septum will achieve stability similar to a columellar strut without the need for graft placement [20].
ii) Onlay tip grafts
Onlay tip grafts are positioned over the alar domes as single or multilayer grafts. They are used to camouflage irregularities or achieve subtle increases in tip projection. Beveling or morselization of the edges minimizes the likelihood of visibility or palpability. An ‘‘umbrella graft’’ is the use of an onlay tip graft in conjunction with a columellar strut where the columellar strut is the umbrella shaft and the onlay tip graft secured to it forms the umbrella top [18]. Placement of tip grafts over the tip-defining points will increase tip projection and definition, whereas placement at and below the tip-defining points will increase projection and add volume to the infratip lobule. It is desirable to secure the grafts within a well-defined pocket.
iii) Shield grafts
These are shield-shaped grafts which are placed over the medial crura, extending from the medial crural footplates to the nasal tip [18]. They are useful in increasing tip projection, defining the nasal tip and enhancing the contour of the infratip region but may leave a visible ‘‘tombstone’’ impression on the overlying skin. They are hence best reserved for patients with thick skin, with edges extensively bevelled or morselized to minimize visibility. The extended shield graft is an ‘‘extended columellar strut-tip graft’’ which extends anteriorly beyond the domes to provide added tip projection[12]. Shield grafts provide the added benefit of derotation of the overrotated nose. The use of conchal cartilage for this graft improves its pliability and confers a softer contour, decreasing the risk for a visible graft silhouette after resolution of oedema.
Grafts of the Alar Region:
Alar batten grafts, alar rim grafts and lateral crural strut grafts are used to increase structural support in cases of overresection or inversion of alar concavities, contour irregularities and rim retractions.
i) Alar batten grafts
These curved cartilaginous grafts of septal or conchal origin used to support areas of maximal lateral wall weakness, usually posterior to the lateral crura. The curvature of the graft is oriented to lateralize the supra-alar area. The grafts may extend beyond the pyriform aperture to add maximal support. When lateral recurvature of the native lateral crura impinges on the nostril width, the lateral crura may be sutured to the alar batten grafts for stabilization laterally. An extended lateral crural strut graft may be used as an alternative when there is significant alar collapse.
ii) Alar rim grafts
These grafts are useful in the prevention or correction of alar retraction and also provide the alae with sufficient rigidity to resist collapse, such as in cases of cephalic malposition of LLC [12]. Additional uses include correction of alar flare and treatment of alar contour irregularity.
iii) Lateral crural struts and lateral crural grafts
These grafts are used when the overall geometry of the nose is projecting, narrow, and thin, with weak cartilaginous support. They provide structural reinforcement of the native lateral crura.
Two types of grafts may be used to achieve this [17]. The lateral crural strut is an underlay graft placed between the vestibular lining and undersurface of the lateral crus whilst the lateral crural graft is an overlay graft placed superficial to the lateral crus.
Grafts of the Nasal Dorsum and Middle Vault
In most cases, the middle vault, the ULCs and the internal valve proper (angle between the ULC and dorsal septum) have less functional airway implications than the lateral wall of the nose but airway obstruction can be significant in noses with a narrow middle vault, a projecting dorsum or inferomedial collapse of the ULC and inverted-V deformity (typically iatrogenic complications from primary rhinoplasty cartilaginous dorsal reduction). Two commonly used grafts of the nasal dorsum and middle vault are described.
i) Spreader grafts (and extended spreader grafts)
Spreader grafts are long rectangular cartilaginous grafts placed between the dorsal cartilaginous septum and ULC to correct problems related to a narrow or asymmetric middle vault. They may be used to reconstruct an “open roof” deformity and to smooth the aesthetic brow-tip line[18]. These grafts may also be used in primary rhinoplasty to prevent ULC collapse, such as when reduction of a cartilaginous dorsal hump leads to excision of the horizontal articulation of the dorsal septum and ULCs. Spreader grafts prevent or correct midvault collapse by stenting open the internal nasal valve, thereby avoiding medial displacement of the ULCs. They therefore stabilize the middle vault and help restore appropriate horizontal width.
ii) Dorsal onlay graft
These grafts are designed to span the entire length of the nasal dorsum, from the radix to the septal angle, to minimize the risk for palpable irregularities. Although septal or conchal cartilage is usually sufficient for refinement of the nasal dorsum, costal cartilage is indicated in those cases where major augmentation is required, for example in severe saddle nose deformity, traumatic compressive fractures, or other major structural deficits.
IV) Dorsal Refinement
The open approach greatly enhances the performance of techniques for dorsal hump refinement. The soft tissue envelope is elevated from the bony-cartilaginous framework up to the level of the nasofrontal angle, taking care to undermine just enough to permit adequate hump reduction and subsequent skin redraping. The authors’ preference is to use an osteotome for larger humps and a rasp for smaller reductions and subtle refinements. Slight undercorrection is preferred, followed by final smoothing with a fine sharp nasal rasp.
Reduction of the septal and ULC components of the dorsal hump may then be done with a no. 11 blade or angled scissors, with or without first separating the ULCs from their attachment to the dorsal septum. If reduction of > 3 mm is desired, submucosal separation of the ULCs before dorsal reduction will preserve the support provided by the nasal mucosa below them. When a lesser reduction is planned, it may generally be performed extramucosally without separating the ULCs from their septal attachment, keeping the nasal mucosa intact. Once the cartilaginous hump is removed, the height of the ULCs relative to the dorsal septum is examined and its medial borders lowered with a no. 11 blade until they lie level with the dorsal septum or the medial part of the cartilage is folded to for an auto-spreader flap.
V) Osteotomies
The potential functional effects of osteotomies on the patient’s nasal airway should always be considered, with the aim to preserve the periosteum and lateral suspensory ligaments of the LLCs.
Osteotomies are indicated:
- To close an open nasal vault
- To straighten a deviated nasal dorsum;
- To narrow the nasal sidewalls.
In general, osteotomies should be limited to the thinner aspect of the nasal sidewall [21] . Commonly used osteotomy techniques include the lateral osteotomy (performed either with a perforation or linear technique), the medial osteotomy and the intermediate osteotomy [22].
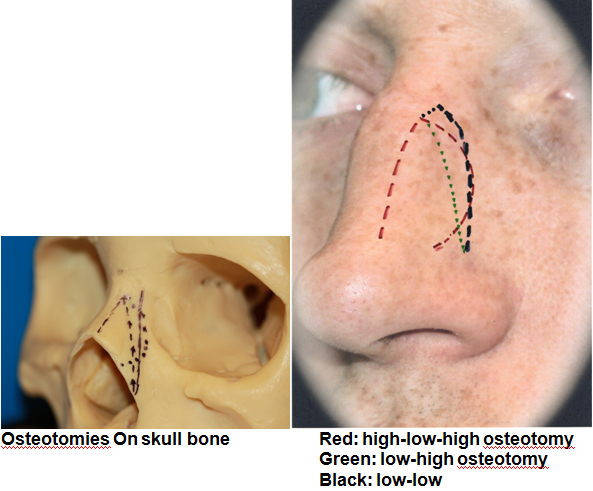
Va) The lateral osteotomy
The lateral osteotomies are performed to close an “open roof” deformity or to narrow the nasal pyramid. This may be performed with either the linear (single-cut) or the perforating technique [9]. With the former, the osteotome is used to make a bony cut along the nasal facial groove. The most widely accepted path of the osteotomy follows a high, low, high pathway [21]. The course of the lateral osteotomy begins at the level of the attachment of the inferior turbinate. A small triangle of bone at the pyriform aperture is left intact to preserve the lateral attachments of the suspensory ligaments. Next, the osteotomy is continued along the nasal facial groove until it curves superiorly and anteriorly into the thinner aspect of the nasal bone at the level of the inferior orbit. The cut is then terminated around the level of the medial canthus [23].
With the perforating technique, a series of perforations using a sharp 2-mm straight osteotome are made along the desired fracture site using a transnasal or transcutaneous approach. With the transcutaneous technique, one or two osteotomy sites are marked on the skin and postage stamp–type perforations are created through these sites along the desired osteotomy route[9]. Alternatively, the perforations can be placed intranasally, such that the perforating intranasal osteotomy can also be used to push out the nasal bones which have been medially displaced by previous trauma or surgery [24] .
The superior backfracture is created by turning the osteotome, applying digital pressure, or using a percutaneous transverse superior osteotomy. In the latter technique, a small cutaneous puncture is created with a 2-mm osteotome midway between the nasal dorsum and the medial canthal region. Through this site, the same osteotome is used to create 3 or 4 small perforations, allowing the nasal bone to be mobilized without disrupting the overlying periosteal support[9].
Vb) The medial osteotomy
Medial osteotomies are used when the nasal sidewalls have to be mobilised, for example when correcting the deviated nose or narrowing the wide nose without a hump. Medial osteotomies are performed in an angulated manner between the nasal bone and septum and are extended superiorly to meet the superior osteotomy site or back-fractured site. In the severely deviated or wide nose, the medial osteotomies are considered essential. When less correction is required, caution is advised as they may actually cause bony irregularities[25].
Vc) The intermediate osteotomy
The main indications are:
- To narrow an extremely wide nose that has good nasal height (bilateral osteotomies)
- To correct a deviated nose with one sidewall much longer than the other,
- To straighten a markedly convex nasal bone[25].
The intermediate osteotomy is made parallel to the lateral osteotomy along the midportion of the nasal sidewall and can be performed more precisely through the open rhinoplasty approach. It is performed before the lateral osteotomy, because the intermediate cut cannot be made easily after the bone is mobilized.
Osteotomies in specific clinical scenarios [25]
1. The extremely deviated nose
The above osteotomies may be used in combination to correct any given anatomic deformity of the bony nasal pyramid. These are performed sequentially beginning on the concave side of the deviation, to allow creation of a space in which to realign the deviation. Camouflage graft techniques are also often essential.
2. Short nasal bones
Palpation of the dorsal nasal hump will often reveal a primarily cartilaginous hump in patients who have short nasal bones. The surgeon must avoid both overmobilization of the nasal bones with osteotomies and overresection of the dorsal nasal bones with a rasp or osteotome. The dorsal hump can sometimes be lowered without performing osteotomies. A perforating osteotomy may be used to preserve maximal soft tissue support. Making a greenstick fracture superiorly is desirable because it also avoids overmobilization of the delicate, short nasal bones.
3. Wide nose
Removal of a significant hump from the wide nose may result in a wide-open dorsum. Standard osteotomies may allow the nasal bones to be moved medially to close the open roof. Debris or residual wedges of bone or cartilage at the junction of the nasal bone and septum must be removed before closure. Bilateral intermediate osteotomies may be necessary to obtain adequate narrowing [25].
VI) Alar Base Narrowing
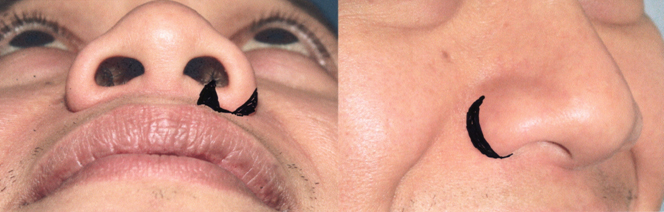
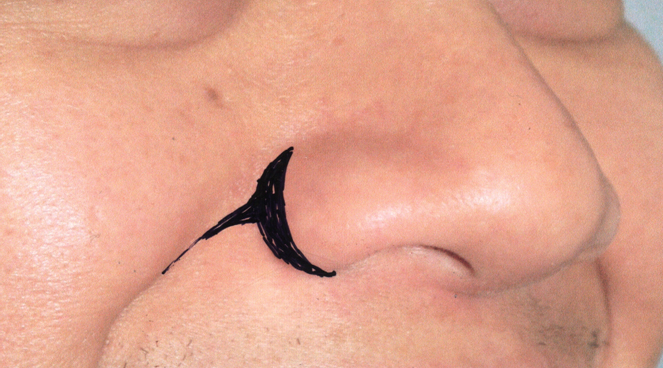
Alar base reduction is best completed as the final step of rhinoplasty often after closure of all incisions. It narrows nasal width, reduces nostril size and alters the nostril axis. A prominent alar flare may be created or worsened by alterations to the lower third of the nose during surgery. Specifically, reduction procedures that decrease tip projection may increase the amount of alar flaring. If there is any doubt at the completion of rhinoplasty that alar reduction is needed, then the procedure should be deferred [26]. The authors feel that reduction of nasal base width should be considered when the interalar distance exceeds the intercanthal distance in the Caucasian patient but ethnic differences and personal preferences should be considered.
The three basic techniques to effect this change are alar base excision, nasal sill excision and V-Y advancement [9, 27]. The goals of alar base excision are to avoid overstraightening the ala, preserve the natural curvature of the ala and avoid telltale incisions into the nostril opening. A wedge resection along the rounded caudal margin of the alar lobule decreases the amount of alar flare. This maneuver may be used together with nasal sill excision, for correction of the excessive flare with enlarged nasal sill width [28]. A relative indication for sill reduction is when the nostril is enlarged and has a horizontal axis [26]. If the lateral insertion of the ala is responsible for excessive nasal base width, then it may be repositioned with a V-Y advancement [29].
Closure
Closure involves careful skin redraping, external contouring, and shaping. The septal mucosal flaps are closed with quilted 4-0 absorbable Vicryl® sutures. To avoid a step deformity of the columella, meticulous closure of the transcolumellar incision with 6-0 Prolene interrupted sutures is vital. As the incision heals, there may be a trapdoor effect of the flap which is most prominent at the junction of the vertical and transverse incision. This can be avoided effectively by undermining the inferior columellar flap.
In cases of reduced nasal projection, there may be excess tissue in the columellar flap, which may lead to columellar hanging. Equally, where the tip has been projected, excessive tension may result due to lack of skin. To reduce this, the vertical margin incision can be bilaterally extended inferiorly to allow the inferior flap to be advanced.
The nasal dorsum is splinted with cheek-to-cheek Steri-strips. A thermoplastic splint is fabricated for additional external support in the perioperative period. No other packing is usually used. The patient is advised to use Fucidin ointment daily to keep the external incision moist.
Followup
Patients are seen at 1 week for suture removal and 1 month postoperatively. Further follow-up visits are scheduled as needed thereafter. At each visit photography is performed.
Complications
Compared to the closed approach, an open approach rhinoplasty carries virtually the same risks, apart from an external scar which usually heals well and remains hidden from view [7]. The risk of complications is higher in revision cases because of scarring and tissue manipulation as summarised below [30] .
Intraoperative complications
- Excessive bleeding
- Tears of mucoperichondrial flaps
- Buttonholing of skin
- Collapse of bony pyramid
- Disarticulation of ULC
- Osteotomy complications
- “Rocker” deformity
- “Open roof” deformity
Early postoperative complications
- Hemorrhage
- Septal hematoma
- Infection
- Persistent oedema
- Skin necrosis
- Sequestra formation
- Olfactory disturbances
Late postoperative complications
- Scar hypertrophy
- Polly beak nasal deformity
- Synechiae formation
- Septal perforation
- Nasal valve collapse
- Vestibular stenosis
- Revision rhinoplasty
Conclusion
The open rhinoplasty approach offers unparalleled exposure of nasal anatomy, structural nasal deformities and is also an invaluable educational tool for the trainee. It allows for precise diagnosis and correction of deformities. These advantages make it a greatly valued technique in the armamentarium of the facial plastic surgeon and ensure its continued usage in the future.
References
1. Rethi, A., Operation to shorten an excessively long nose. Rev Chir Plast, 1934(2): p. 85-7.
2. Sercer, A., [Nasal decortication and its value in cosmetic surgery]. Rev Laryngol Otol Rhinol (Bord), 1957. 78(3-4): p. 161-8.
3. Padovan, T., External approach in rhinoplasty (decortication). Symp ORL, 1966(4): p. 354.
4. Anderson, J.R., C.M. Johnson, Jr., and P. Adamson, Open rhinoplasty: an assessment. Otolaryngol Head Neck Surg, 1982. 90(2): p. 272-4.
5. Wright, W.K. and R.W. Kridel, External septorhinoplasty: a tool for teaching and for improved results. Laryngoscope, 1981. 91(6): p. 945-51.
6. Gunter, J.P., The merits of the open approach in rhinoplasty. Plast Reconstr Surg, 1997. 99(3): p. 863-7.
7. Sheen, J.H., Closed versus open rhinoplasty–and the debate goes on. Plast Reconstr Surg, 1997. 99(3): p. 859-62.
8. Adamson, P.A. and S.K. Galli, Rhinoplasty approaches: current state of the art. Arch Facial Plast Surg, 2005. 7(1): p. 32-7.
9. Adamson, P.a.L., J., Open rhinoplasty, in Facial Plastic and Reconstructive Surgery, I. Papel, Editor. 2009, Thieme. p. 529-47.
10. Mangat, D.S. and B.J. Smith, Septoplasty via the open approach. Facial Plast Surg, 1988. 5(2): p. 161-6.
11. Whitaker, E.G. and C.M. Johnson, Jr., The evolution of open structure rhinoplasty. Arch Facial Plast Surg, 2003. 5(4): p. 291-300.
12. Smith, T.W., Thoughtful nasal tip surgery. Arch Otolaryngol, 1973. 97(3): p. 244-6.
13. Murakami, C.S., J.E. Barrera, and S.P. Most, Preserving structural integrity of the alar cartilage in aesthetic rhinoplasty using a cephalic turn-in flap. Arch Facial Plast Surg, 2009. 11(2): p. 126-8.
14. Tardy, M.E., Jr., B.S. Patt, and M.A. Walter, Transdomal suture refinement of the nasal tip: long-term outcomes.Facial Plast Surg, 1993. 9(4): p. 275-84.
15. Simons, R.L., Vertical dome division in rhinoplasty. Otolaryngol Clin North Am, 1987. 20(4): p. 785-96.
16. Tardy, M.E., Jr., J. Denneny, 3rd, and M.H. Fritsch, The versatile cartilage autograft in reconstruction of the nose and face. Laryngoscope, 1985. 95(5): p. 523-33.
17. Kridel, R.W. and R.J. Konior, Controlled nasal tip rotation via the lateral crural overlay technique. Arch Otolaryngol Head Neck Surg, 1991. 117(4): p. 411-5.
18. Brenner, M.J. and P.A. Hilger, Grafting in rhinoplasty. Facial Plast Surg Clin North Am, 2009. 17(1): p. 91-113, vii.
19. Conrad, K., C.S. Torgerson, and G.S. Gillman, Applications of Gore-Tex implants in rhinoplasty reexamined after 17 years. Arch Facial Plast Surg, 2008. 10(4): p. 224-31.
20. Johnson, C.M., Jr. and Toriumi, DM, Open Structure Rhinoplasty. 1990: WB Saunders. 516.
21. Larrabee, W.F., Jr. and C. Murakami, Osteotomy techniques to correct posttraumatic deviation of the nasal pyramid: a technical note. J Craniomaxillofac Trauma, 2000. 6(1): p. 43-7.
22. Aufricht, G., Joseph’s rhinoplasty with some modifications. Surg Clin North Am, 1971. 51(2): p. 299-316.
23. Anderson, J.R., A new approach to rhinoplasty. Trans Am Acad Ophthalmol Otolaryngol, 1966. 70(2): p. 183-92.
24. Rohrich, R.J., et al., The lateral nasal osteotomy in rhinoplasty: an anatomic endoscopic comparison of the external versus the internal approach. Plast Reconstr Surg, 1997. 99(5): p. 1309-12; discussion 1313.
25. Larrabee, W., Open rhinoplasty and the upper third of the nose. Facial Plast Surg Clin North Amer, 1993(1): p. 23-38.
26. Kridel, R.W. and R.D. Castellano, A simplified approach to alar base reduction: a review of 124 patients over 20 years. Arch Facial Plast Surg, 2005. 7(2): p. 81-93.
27. Weir, R.F., On restoring sunken noses without scarring the face. 1892. Aesthetic Plast Surg, 1988. 12(4): p. 203-6.
28. Aufricht, G., Rhinoplasty and the face. Plast Reconstr Surg, 1969. 43(3): p. 219-30.
29. Bernstein, L., Esthetic anatomy of the nose. Laryngoscope, 1972. 82(7): p. 1323-30.
30. Cochran, C.S. and A. Landecker, Prevention and management of rhinoplasty complications. Plast Reconstr Surg, 2008. 122(2): p. 60e-7e.
